
Before I grab my coffee and head out for the site.
June 12, 2020
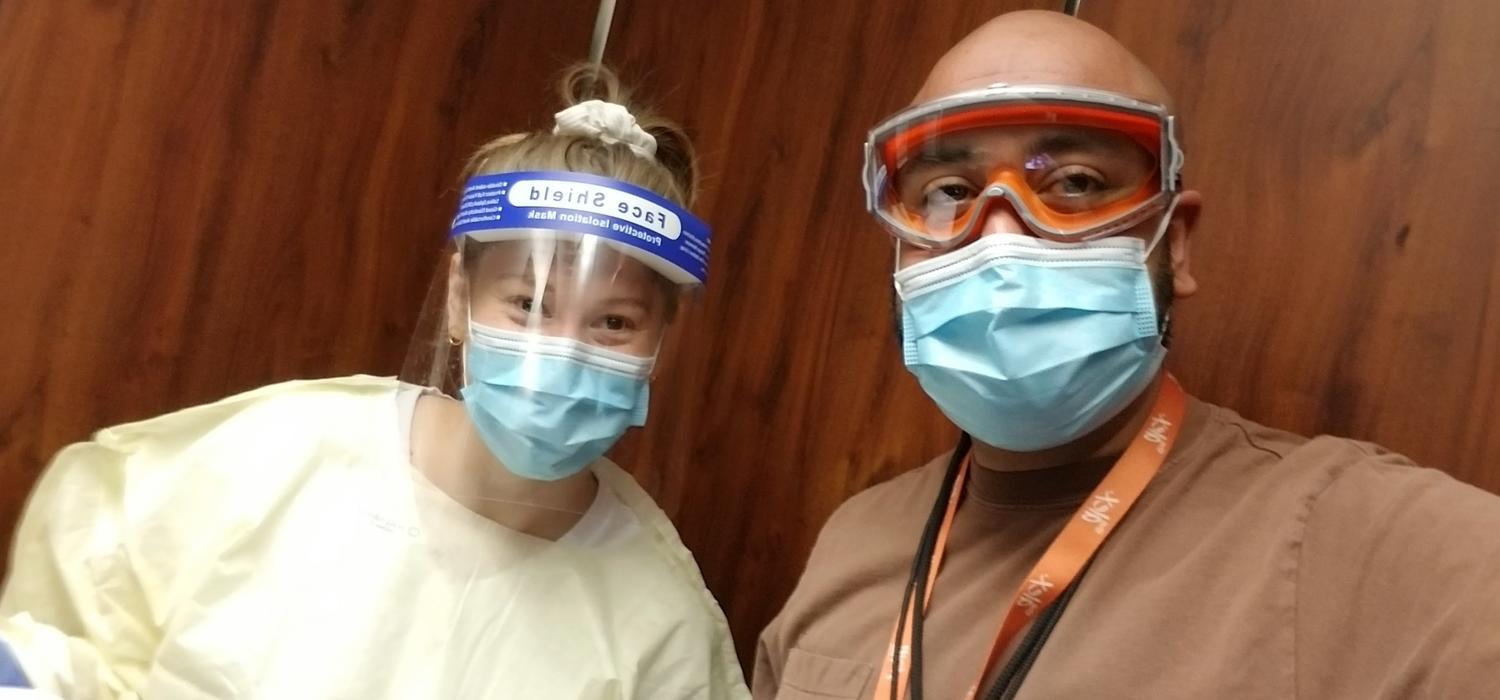
On Friday, March 13th this year, my class found out year one med school OSCE* examinations were cancelled due to an increasing abundance of caution surrounding COVID-19. Our longest vacation break would be in the age of social distancing, and, as someone who wears two hats — I am an RN and a medical student — I became restless searching for ways to help with the pandemic.
*OSCE – Objective Structured Clinical Examination are exams often used in health sciences
In the early weeks, I remotely loaned some expertise to colleagues at The Alex, Alberta Health Services (AHS) and Calgary Rural Primary Care Network, and used the time to adjust and sort through the upcoming curriculum changes for myself. All the while, I was compelled to continue reaching out to my RN colleagues looking for a way to help on the frontline however I could. My mentor and old friend, an RN and health director at The Alex, called me one day in April with the opportunity in hand.
Partnerships in the community between a property owner, municipal government, the Calgary Homeless Foundation and The Alex had resulted in the creation of a “pop-up isolation shelter” to serve our city’s homeless during COVID-19. AHS came on board early, demonstrating strong inter-sectoral collaboration for health to address gaps that are primary and upstream.
The innovative project was envisioned in part to answer a question that was nagging me the whole time: During the age of social distancing and COVID-19, how do you stay at home if you are homeless?

Before I grab my coffee and head out for the site.
Once again, the social sector stepped up and led the way in creating the Assisted Self-Isolation Site (ASIS), which you can read about in The Calgary Herald. By April 25th, as the province made plans to begin re-opening, the first positive COVID-19 cases turned up at the Drop-In Centre. The need in our city would rapidly become much greater over the coming weeks.
RNs are in higher levels of leadership at the site, creating and implementing innovative health and social care for a very vulnerable population. I get to perform health assessments and intake screenings, monitor for ongoing concerns such as substance withdrawal management, while coordinating social supports and ensuring the primary care providers (NPs and MDs) are knowledgeable about their patients’ pressing health concerns. We create policies and procedures “on the fly,” adapting and changing them on a daily basis. The speed of change can be exciting, overwhelming, or both. We participate in contact tracing and swabbing for COVID-19, managing clients in a cohort fashion who are positive, negative, or pending test results.
Our social team is essential in planning for housing when clients leave, and/or setting them up with an addiction treatment program. We practice harm reduction and housing first principles, assessing for acuity and providing medical support if needed. It requires navigating the importance of client autonomy, public health requirements for isolating close contacts of COVID-19, and professional ethics to provide care when necessary and able.
The site has fewer resources available than hospitals, so it relies on the combined wisdom of many veteran health-care workers from the homeless sector.

Early orientation days at the site with Heather Brooks (LPN, ACP, ORT).
I work alongside the most intelligent, adaptable, and compassionate LPNs, NPs, MDs, pharmacists, social workers and addiction specialists in the city. Most of my clinical training for the site involved being targeted in my approach. Highly knowledgeable and experienced LPNs taught me this in the early stages and are leaders in the nursing group. The case workers and addiction specialists continue to teach me something new about client engagement every day.
It is a work culture where colleagues are treated as equals, bringing their scopes of practice, unique skill sets and experiences to a team with common goals. It is interdisciplinary work also by way of individuals having strong cross-training. For example, I learned a lot from an advanced-care paramedic who earned her LPN licence while continuing to work. Others include RNs and MDs with social work or psychology backgrounds, and a handful with a Master’s in Public Health. Almost everyone has some background in mental health, or would like to gain some.
The staff at the site have various backgrounds in their work environments, too: from urgent care to ICU, rural hospitals and mental health facilities, to assertive community treatment teams and forensic/incarceration settings. Nursing students who I taught as a lecturer at UCalgary are now my colleagues at ASIS.
I remember my first exposure to The Alex as a BN student myself, in 2012. The early years are formative, and it has been rewarding to find my interactions with students at an early stage influenced their thoughts on where RNs can work, and their potential impact in community health nursing.
Most of the RNs on site have been re-deployed from other locations or leaves of absence, demonstrating versatility in the profession to be able to go where the need is greatest, and a scope of practice that is far-reaching. I even met a fellow medical student a year ahead of me, herself an RN, just by chance working there.
Soon after I started working, other nurses in medical school reached out to me about helping at ASIS, if they were not already re-deployed in their home settings of ICU or otherwise. I have been moved and affirmed in my belief that you never stop being a nurse.
I am lucky to be an RN, able to help out at the frontline. Many health-care students have felt unable to help, often juggling complicated feelings as they make their way through online studies in an uncertain time. My classmate and fellow social justice advocate wrote about some of these shared struggles for CBC Calgary. The perspective is of a medical student, but I think it resonates with nursing students as well.
Taking a strengths-based view (which we promote in nursing) would demand acknowledgment of how amazing health-care students in all faculties have been during this time: leading the way on contact tracing, providing childcare for frontline workers, creating seniors’ programs to help with medication and grocery deliveries, and supporting each others’ mental health — among so many other initiatives.
Many young students have demonstrated resilience in the face of uncertain curricular developments, choosing to help however they can, rather than focus on their individual concerns. They have recognized how communal this event truly is. No matter where someone is in their health-care career, their time, effort and expertise have been utilized during COVID-19.

From top to bottom: Rachel Tenszen RN BN, Jenaye Kinakin RN BN, and Hailee Crawford RN BN - all BN grads of UCalgary's Class of 2020.
And likely this will not be their last opportunity to be involved at the frontline during a major event. So, it is important to study! Students should not feel guilt if their job right now is to be a student.
I have had to dial back my own clinical involvement, to make sure that I do well at school. I am looking forward to another role transition while continuing similar work, if I keep up my studies. I witnessed something awesome during my time at ASIS: three case support workers were working there diligently supporting our clients and ASIS operations. I found out they had written their NCLEX exams as BN graduates. They have since passed and are transitioning to the nursing team as RNs! Part of my ongoing professional development involves staying grounded in the work by young professionals, who keep me in check when I start to slack off in my practice.
I am optimistic after seeing the innovation, compassion, and determination of our health-care workers to meet the challenge of COVID-19. I believe our future health-care practitioners will be even brighter and more empathetic to meet similar challenges, which are likely to come.
Heartfelt thanks go to my 'holy trinity' at the ASIS site: Jennifer Eyford, Rachael Edwards and Danielle Szabo. You helped me be a small part of something incredible.
Sekhon graduated with his BN from the Faculty of Nursing in 2014 and his MN (thesis) in 2019. He was featured as one of our “50 Faces of Nursing” in 2019. He has worked clinically with The Alex, Calgary Rural Primary Care Network, as well as Alberta Health Services in acute care settings. He served as a guest lecturer and sessional clinical instructor for Community Health Nursing, especially for topics in addiction and mental health. Currently he is working toward completing his MD with the Cumming School of Medicine (Class of 2022 – Tanuki).