
Prism Schneider and Kaitlyn Dillabough are creating resources for health-care providers.
Don Molyneaux
March 19, 2020
One in six women has experienced intimate partner violence in the last 12 months. One in 50 women seen at an orthopedic clinic has an injury caused by intimate partner violence.
A recent study on intimate partner violence and orthopedics reveals the high prevalence of intimate partner violence (IPV) patients seen in fracture clinics within Canada. The study looked at 12 centres, including Calgary, and over 3,000 patients.
The findings of the study present an opportunity for orthopaedic clinics to identify and provide resources and education for both victims and perpetrators of intimate partner violence.
McCaig Institute member Dr. Prism Schneider, MD, PhD, and master’s student Kaitlyn Dillabough are creating learning resources and developing screening tools for health-care professionals to break the cycle of intimate partner violence.
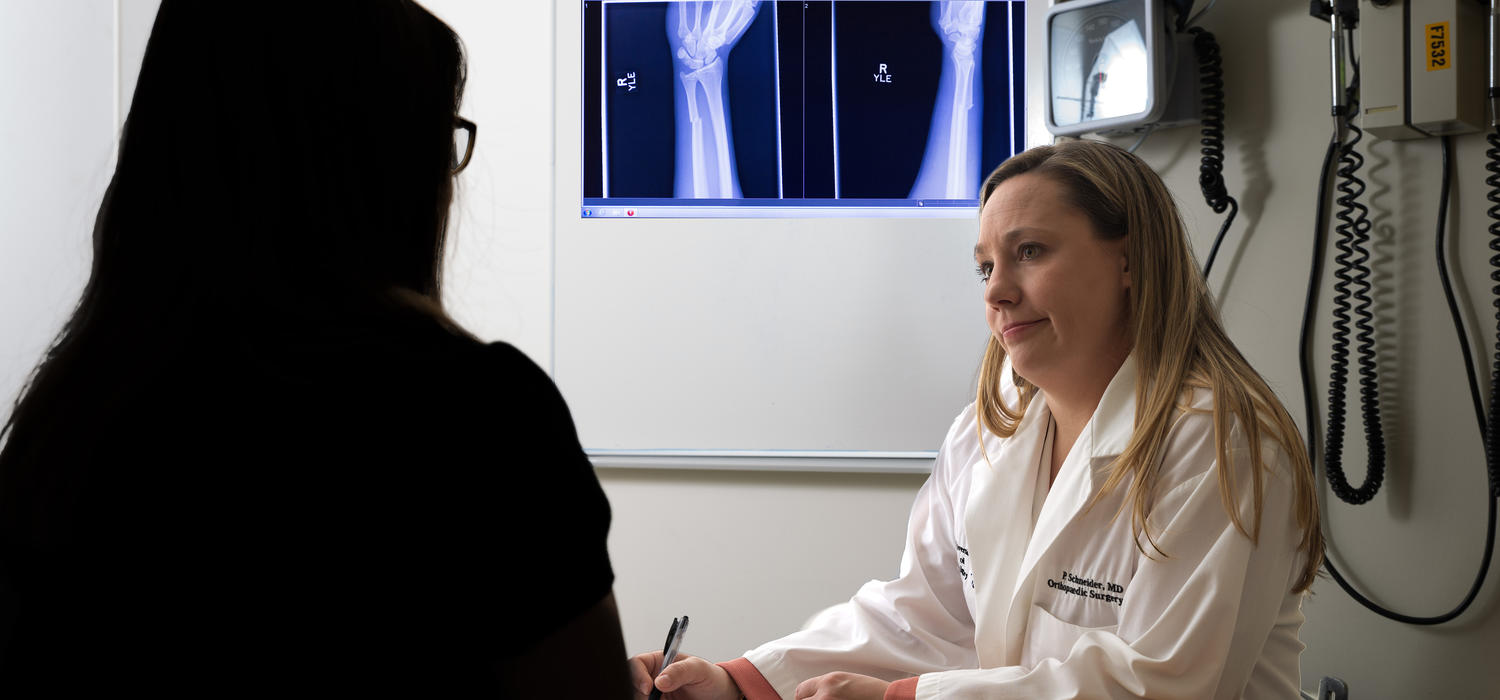
“Unfortunately, I care for a large number of patients with significant injuries due to violent relationships. My ultimate goal is injury prevention and awareness, so when victims of IPV are seen by health-care professionals, we are able to identify those patients and provide help not only for them, but also to their partners to prevent further injury and even death,” says Schneider, MD’08, PhD’08, pictured above with a patient.
Schneider has transformed her own practice in hopes of breaking the cycle of intimate partner violence and ending stigmatization. She is using routine visits to build rapport with each patient. She asks every female patient at every appointment about their safety at home to open a dialogue, so if they are in an unhealthy relationship, she will be able to intervene and provide resources to them.
Her patients have been very responsive to the change in conversation. “We can no longer sweep these issues under the carpet; asking about IPV should be as normal as asking for someone’s address,” says an anonymous patient.
“Intimate partner violence occurs across every gender, every relationship type, and socioeconomic status. This understanding helps us adopt a new philosophy of asking every patient, in order to normalize this conversation and create a new patient experience,” says Schneider.
Since transforming her own patient care routine, Schneider is starting to notice a shift at her clinic. In the past, screening practices and suspicions of IPV were often ignored, largely due to a lack of knowledge and resources on how to help.

Prism Schneider and Kaitlyn Dillabough are creating resources for health-care providers.
Don Molyneaux
MEDUCATE program
“In medical school, we learn how to identify different injuries and fracture patterns that may signal abuse; however, there is little additional training on what to do or how to intervene when suspicions of IPV are present,” says Schneider.
Identifying a need for awareness and IPV education, Schneider and Dillabough launched the first MEDUCATE program for 25 medical students at the Cumming School of Medicine (CSM).
As a pilot program, modeled after the EDUCATE program created by McMaster University, Schneider and Dillabough offered an evening workshop on IPV. The workshop offered students an opportunity to practise conversations with an actor portraying a patient, complete with feedback provided by their peers and a social worker.
Feedback from the session was resoundingly positive, with participants valuing the opportunity to become more comfortable with the issue of IPV. Students who participated will become physicians in many different areas of medicine, so Schneider and Dillabough are hopeful that they will bring awareness, knowledge, and practice to their areas of specialization. They plan to lead another workshop this year.

Prism Schneider and Kaitlyn Dillabough are creating resources for health-care providers.
Don Molyneaux
Typically, IPV screening focuses on identifying victims; however, Schneider and Dillabough are shedding light on the importance of intervention for the perpetrators of IPV in their current project: VIVIR (Validating a Tool for Use in Identifying and Assisting those in Violent Intimate Relationships).
“It is very likely that we are seeing perpetrators of IPV in clinics and it is important that health-care providers have resources to screen for perpetrators in order to provide resources and break the cycle of abuse,” explains Dillabough.
Past questionnaires for screening perpetrators were lengthy, with many containing accusatory language. The aim of the VIVR project is to create a revised questionnaire with acceptable language for both patients and health-care providers, with the goal of developing an effective and non-judgmental screening tool for orthopedic clinics and other medical settings.
“My hope for this project and future research is to increase awareness about IPV and to create tools that provide health-care professionals with resources in a multitude of settings to identify and assist not only victims, but also the perpetrators of IPV,” says Dillabough.
The 24/7 gateway number for patients and the community is 403-234-SAFE (7233). Anyone can call with a concern and they will be directed to the appropriate resource and support.
Kaitlyn Dillabough is a first year master’s student in the medical sciences program at the CSM. Dillabough has also completed a Bachelor of Science in Health Sciences from Mount Royal University.
Prism Schneider is an orthopedic trauma surgeon and a clinical associate professor in the departments of Surgery and Community Health Sciences at the CSM. She is a member of the McCaig Institute for Bone and Joint Health and a member of the O’Brien Institute for Public Health.